Treatment options for liver disease are currently limited, but a readily available source of primary human hepatocytes could revolutionize this field. Primary human hepatocytes, or liver cells, have been shown to be effective in the treatment of acute, chronic and rare forms of liver disease. With a reliable and consistent supply of primary hepatocytes, we can advance the understanding of liver diseases, enable new therapeutic applications and provide a better source of cells for current uses in toxicology and metabolic safety studies for drug development.

In healthy humans, the liver is continually regenerating in order to carry out many critical functions that keep us alive and well.

What if we could harness the enormous regenerative power of the liver to treat people whose livers have lost that innate capacity?
Hepatocytes are cells produced by the liver that are responsible for liver regeneration and, as a result, key liver functions.
The loss of hepatocytes or hepatocyte function is the primary cause of liver failure.
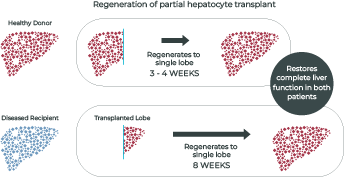
Unlike liver transplant which replaces a patient’s whole organ, our cell therapy approach harnesses the regenerative power of healthy hepatocytes to accelerate the healing process. Whether utilized directly through cell transplantation or incorporated into an external bioartificial liver, our high-quality and abundant supply of healthy hepatocytes offer a better solution for restoring liver function and improving patient outcomes.
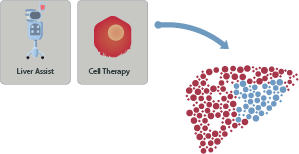
Cytotheryx specializes in manufacturing clinical-grade, scalable Primary Human Hepatocytes, facilitating therapeutic innovations in bioartificial liver technologies and hepatocyte replacement therapies, aimed at bridging patients to transplant and/or restoring optimal liver function.
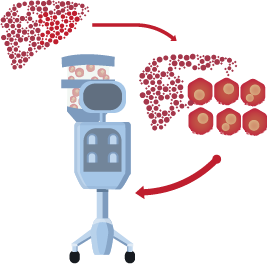
Through advancements in research demonstrating the utilization of hepatocytes, we are pioneering the development of a Bioartificial Liver that harnesses the power of Primary Hepatocytes as a biological component to filter and detoxify patients’ blood. This innovative therapy will offer a revolutionary approach, bridging patients to transplants or recovery.
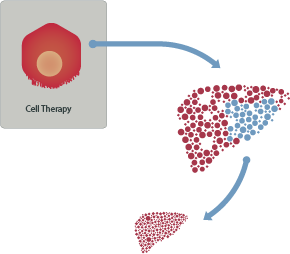
We are also advancing a direct hepatocyte transplantation therapy. Our allogeneic, or ‘off-the-shelf,’ cell therapy will deliver a universal, healthy human hepatocyte to patients with rare, chronic, and acute forms of liver disease.
